Private health exchange an attractive option as enrollment doubles
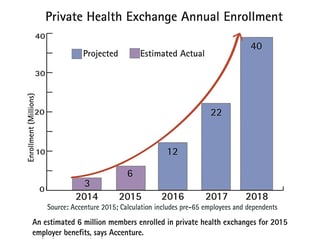
CHICAGO — The online marketplace for private health insurance exchanges doubled enrollment this year to 6 million covered, according to a report by Accenture released Tuesday.
Based on its research, Accenture forecasts that enrollment in private health insurance exchanges will grow to 12 million in 2016 and 22 million in 2017. As previously forecasted, Accenture expects total enrollment in private exchanges to ultimately surpass state and federally funded exchanges, reaching 40 million by 2018.
“We remain optimistic that several factors will catalyze enrollment growth in private health insurance exchanges through 2018," said Rich Birhanzel, managing director for Accenture Health Administration Services. “This is especially true as the market matures, employers gain more control of benefit design and evidence continues mounting on the tangible benefits of the model.”
Accenture’s findings show midsize employers, defined as companies with 100 to 2,500 employees, contributed most to the adoption of private health exchanges increase.
According to Accenture, many employers did not drop coverage in 2015, as initially forecasted. In fact, an Accenture survey found that 76% of consumers with employer-sponsored coverage see health insurance as a primary factor for continuing to work at their current employer, limiting some employers’ ability to drop or defund health coverage. As employers seek a compelling alternative, private exchanges will emerge for some as a compelling model to reduce costs and administrative burden.
Private exchange enrollment is expected to accelerate in 2017 due to looming penalties for “Cadillac” Plans. This provision of the Affordable Care Act places a 40% excise tax on high-cost employer health plans beginning in 2018. Research estimates that 38% of large employers (those with more than 2,500 employees) and 17% of American businesses overall will face those penalties in 2018 if action is not taken prior.
Other factors driving growth of private health insurance exchanges include continued investments by exchange sponsors in private exchange technology solutions, such as Aetna’s acquisition of bswift and Mercer’s equity investment in Benefitfocus, are expected to drive market maturity and scalability.
And the number of large employers who have been on the fence in determining whether to adopt private health insurance exchanges is expected to drop over the next two years due to looming mandates and a maturing market, Accenture added. In addition, Accenture expects that increased compliance requirements mandated by regulations, such as the ACA (section 6055), HIPPA and the Employee Retirement Income Security Act, will drive employers to adopt new models for managing benefits administration.