Diabetes management gets some high-tech help
People living with diabetes will tell you it’s a full-time job understanding how their body will respond to different foods and how stress, exercise, environmental factors and even routine daily activities cause them to readjust their insulin and glucose intake multiple times a day.
And for children living with this condition, their caretakers must think about all of these things and learn their insulin needs for them.
Now layer on top of this the expense of living with this autoimmune disease. The diabetes research foundation JDRF estimates adults with Type 1 diabetes spend about $20,000 a year managing their condition.
[Read more: Lannett completes clinical trial subject dosing of biosimilar insulin glargine]
Fortunately, the number and quality of options for diabetics has increased dramatically. Today’s diabetics can lead healthier, fuller lives thanks to new user-friendly, affordable and discrete devices that have been developed to assist them with daily self-care routines and needs.
The reasoning behind the advances in delivery and monitoring equipment can be distilled into two words: improving compliance. As the number of people diagnosed with diabetes has risen each year, compliance has headed in the opposite direction. Diabetics describe the older methods as being cumbersome, painful, complicated and unreliable at times.
Hearing this, manufacturers have been delving into how they can remediate these issues. The answer, they discovered, is technology. The result has been the introduction of cutting-edge tech, such as closed loop systems, smaller and more accurate continuous glucose monitors, smart devices and faster-acting insulins. What’s more, during the next few years, as costs come down and nano technology enables the hardware to be miniaturized, more advancements are expected.
Challenges and issues
Insulin pump therapy has historically been expensive and difficult to access, said Bret Christensen, chief commercial officer at Acton, Mass.-based Insulet. To address this, Insulet’s products are available at the pharmacy, which means most customers pay less than $50 per month with no commitment, and they can get their pump supplies at the same place they get their insulin. “It’s more convenient and more affordable than the Durable Medical Equipment benefit, which is how all other insulin pumps are covered by payers,” he said.
Many patients, Christensen noted, are struggling with the burden of diabetes, explaining that daily tasks, such as checking blood sugars and delivering insulin, can be overwhelming, not to mention diminish a person’s quality of life. “Pharmacy organizations and pharmacists are in a unique position to help identify patients who need help with their diabetes care and create more awareness of technologies, such as continuous glucose monitoring and insulin pumps available through the pharmacy,” he said.
[Read more: Optum to offer lower-cost Sanofi insulin for uninsured people with diabetes]
Christensen added that “evidence suggests these technologies can improve outcomes and lessen the burden of diabetes. With medication adherence as one of the primary roles of a pharmacist, they stand to play a critical part in the healthcare continuum.”
Advanced in monitoring
Blood glucose monitoring, or BGM, has been used for decades and remains an important tool in diabetes management, but BGM has its limitations, said Chris Scoggins, vice president of commercial operations and marketing at Abbott’s Diabetes Care Business, based in Abbott Park, Ill. “BGM requires painful fingersticks and can only provide point-in-time information,” he said. “High and low blood glucose fluctuations can often go undetected — even when people are performing multiple daily fingersticks.”
Continuous glucose monitoring systems were designed to address these issues and have been life changing for millions of people. Advancements in CGM technology have led to next-generation devices that are more accurate, discreet, easier to use and connected to apps with compatible smartphones.
[Read more: Enhancing diabetes prevention and care services]
“CGM allows people living with diabetes to automatically track their glucose levels day and night,” Scoggins said. “Through a smartphone app or reader, people can see where their glucose values have been, where they are now and where they are going through use of trend arrows.”
Emory Anderson, president and CEO of Intuity Medical, located in Fremont, Calif., pointed out that people with diabetes have been frustrated with options to date and the disruption it presents to everyday life. Given the limited innovation with BGM, patients are clamoring for something much simpler, Anderson said.
Solutions
Medtronic’s solution to simplifying and streamlining insulin delivery was to introduce a smart pen. The company’s next goal is to increase availability of this device. “Smart, connected devices automatically capture dose information, alert for missed doses and provide individualized dosing decision support,” said Janice MacLeod, director of clinical advocacy, global professional affairs and clinical education at Medtronic Diabetes, located in Northridge, Calif.
“These features play a key role in modernizing care for a large population of people on insulin injection therapy and support evolving care models that are moving to asynchronous continuous care with remote data monitoring.” By recognizing the disparities that exist in diabetes technology access and ongoing use, extending technology options to a broader population is critical, she said.
[Read more: Diabetes care goes beyond medical devices]
What’s more, when paired with specific apps, smart devices play an important role in collecting and sharing patient-generated health data. “Shared data opens the door to remote monitoring and more frequent, personalized, continuous care models that can be efficient for both the patient and the provider. Diabetes is a data-driven, chronic condition that requires the patient to make decisions daily about their self-care,” MacLeod said. “Technology solutions empower them to make the best decisions and give them the ability to share data with their care team so they can collaborate to optimize the care plan on a timely basis.”
Medtronic’s InPen provides a customizable fast-acting insulin therapy solution for people with Type 1 or Type 2 insulin-dependent diabetes. InPen provides a choice of therapy modes: carb counting, fixed dose and meal estimation dose calculators to those who use multiple daily injections based on their healthcare provider’s recommendations. “This puts actionable diabetes treatment suggestions into the hands of users and healthcare providers, no matter the insulin treatment protocol,” MacLeoduo said. With real-time glucose data from the Guardian Connect CGM in the InPen app, patients can see their glucose, active insulin and dosing recommendations — all in one convenient view.
Insulet’s latest innovation in insulin delivery is an Automated Insulin Delivery (AID) system. According to Christensen, the AID system integrates both insulin pump and CGM technology to deliver dynamic insulin adjustments in response to real-time glucose measurements to minimize hypoglycemia and hyperglycemia. “The Omnipod 5 System is the only tubeless automated insulin delivery system integrated with Dexcom G6 CGM to manage blood glucose with no multiple daily injections, zero fingersticks, and is fully controlled by a compatible personal smartphone,” he said.
[Read more: Abbott’s FreeStyle Libre 3 approved by FDA]
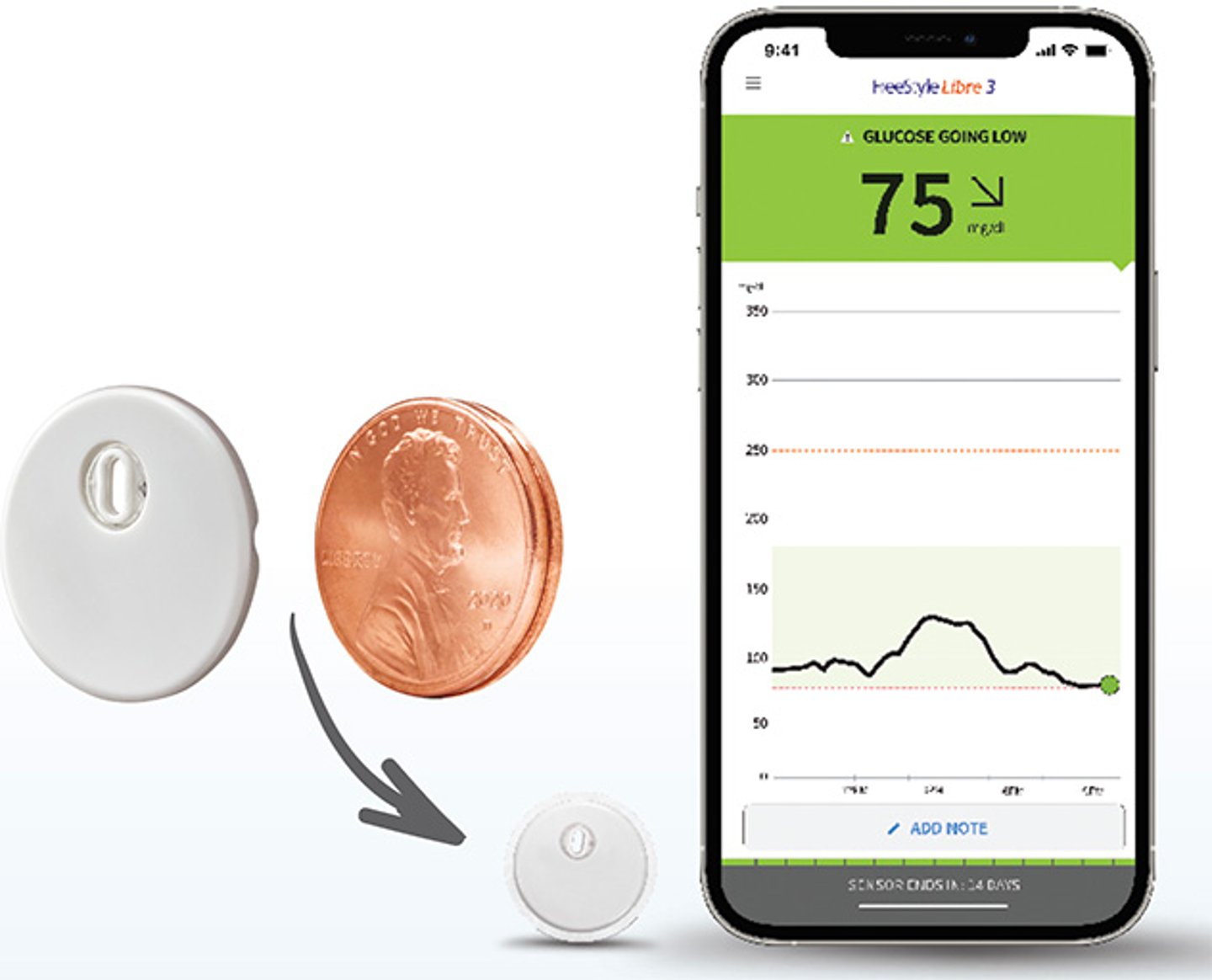
With its latest FreeStyle Libre 3 system, Abbott created the smallest, thinnest and most discreet on-body sensor on the market — about the size of two stacked pennies. The system automatically sends real-time, minute-by-minute glucose readings to a compatible smartphone without scanning, has the strongest Bluetooth range of any CGM and uses significantly less plastic than previous versions. This technology offers optional glucose alarms beyond mandatory ones and provides glucose history and trend arrows with a quick look at your phone.
Additionally, it integrates with LibreLinkUp (smartphone app) and LibreView (cloud-based data system), enabling caregivers and healthcare professionals to monitor loved ones and patients remotely. “This technology gives people living with diabetes more freedom and less pain,” Scoggins said. “ It’s a game changer for the millions of people living with diabetes.”
While there has been a lot of innovation happening around diabetes data management, new therapies, digital therapeutics and CGM over the last several years, currently CGM is only used by a limited segment of the population with diabetes, according to Anderson. “That’s why it’s great to be able to bring a technology like automatic blood glucose monitoring — or ABGM — to the conversation because it’s a technology that enables the entire population with diabetes to get in on the excitement around diabetes innovation,” he noted.
[Read more: Diabetes goes digital: Innovative technologies are revolutionizing diabetes care and monitoring]
Anderson said ABGM represents innovation that understands the burdens people with diabetes still face and gives them another way to meet their blood glucose testing needs. He predicted that we will see more of that kind of innovation in the future — innovation with broad application across the category.
Intuity Medical recently introduced POGO Automatic, the first and only FDA-cleared ABGM whose 10-test cartridge technology makes it possible to lance, collect blood and produce a glucose result in just one step, without the need to individually load lancets or test strips. “With One-Step testing, POGO Automatic delivers a greatly simplified and discreet blood glucose testing experience that is less disruptive to the everyday lives of people with diabetes,” Anderson said.
Future
When Abbott created the FreeStyle Libre technology, the company said it always knew it could be used for more than glucose and could reach beyond people with diabetes, Scoggins said. While glucose remains a priority, the company is currently developing the technology to go beyond this. For instance, Abbott is developing a bio-wearable device that measures both glucose and ketones in the same sensor.
Abbott is also working on consumer bio-wearables for people without diabetes, designed to track key biomarkers, such as glucose, ketones and lactate, to give people real-time data and personalized insights to help them improve their general health and wellness.